Compassion is one of the core values that care workers should embody – but just what is compassion in health and social care? And how can you ensure that you’re doing the right thing for your clients, especially when you’re rushed, stressed, and trying to support other people as well?
Every care worker should strive to be compassionate. They should try to make their clients comfortable, ease their distress, and improve their quality of life. But it isn’t always easy.
In this article, we’ll look at what compassion means, and some barriers that make it harder to be compassionate. We’ll also talk about how you can improve compassion within your care service.

Table of Contents
What are the 6 Cs in health and social care?
The 6 Cs in health and social care are a set of key values that all care workers should attempt to embody. They are:
- compassion (which we’ll be looking into more detail today)
- care
- competence
- communication
- courage
- commitment
Book a free tour
Turn compassion into consistent care
See how PASS helps care teams capture individual needs, share updates in real time, and stay aligned, so every person receives thoughtful, person-centred care.
From clear care plans and shared notes to real-time oversight, PASS gives your team the tools to deliver compassionate care every day, while reducing admin and improving communication.

Compassion meaning
Compassion means feeling sympathy for people who are suffering. Compassionate people want to support those who are in pain or discomfort, and help them to feel better.
They’re often proactive, and try to solve problems – but also understand that sometimes, they just need to listen and be a good companion.
Some people are naturally very compassionate, whereas others might need to learn the right behaviour over time.
How can we show compassion in social care?
So, just what is compassion in health and social care? If you’re a carer, you probably show compassion to your clients in lots of different ways each shift – even if you don’t realise it.
Some examples of compassion might include:
- Learning your client’s preferences and wishes – for example, remembering how they take their tea or want their hair styled.
- Respecting your client’s dignity – for example, giving them privacy by closing doors and curtains before providing intimate care.
- Being patient with clients – for example, letting someone with a stammer finish their sentence rather than interrupting them.
- Listening to your clients – for example, spending some extra time talking with a client and providing companionship, rather than just delivering personal care.
To be a compassionate care worker, keep asking yourself: “How can I make my client feel better?”
Barriers to compassion in health and social care
As a care provider, you know that you should always be compassionate towards your clients. However, it isn’t always that easy.
There are some barriers that can make it harder to show compassion, such as time constraints, personality clashes, and even carer burnout.
Let’s look at some examples of barriers to compassion, along with potential solutions.
Time constraints
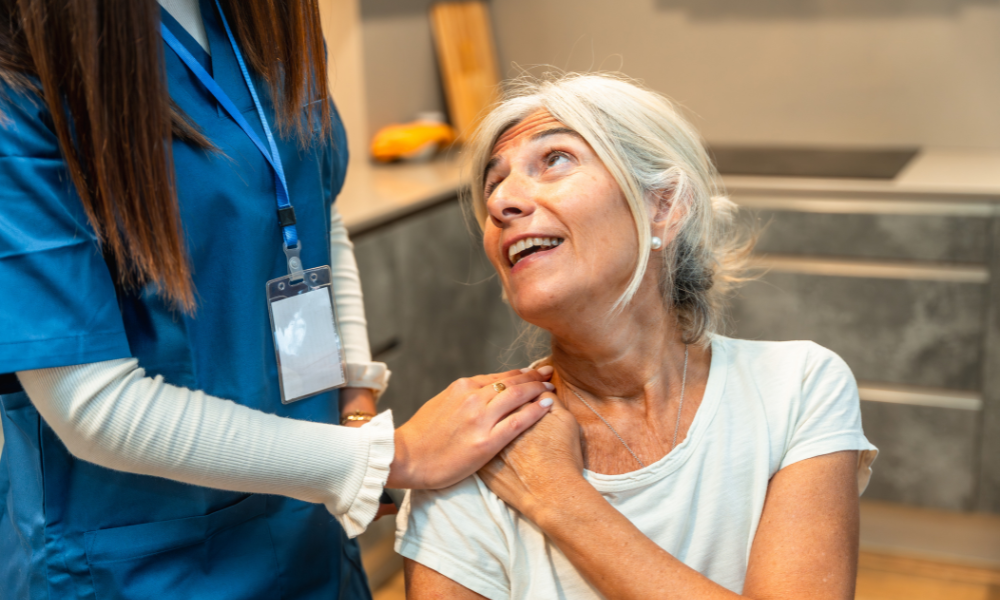
Most care agencies and residential facilities have very tight schedules.
Care visits may be very short – once you’ve helped your client wash, dress, and take their medication, there might not be time left over for a chat.
Unfortunately, these tight schedules and time constraints can make care workers less compassionate. If care visits are too short, carers will naturally be worried about timing, and might try to rush clients. They may ignore opportunities to listen, and they might even be tempted to cut corners and take away a client’s freedom to choose.
Example:
John works in a care home, and delivers care to four clients each morning. His first client, Matthew, needs support with washing, dressing, and taking his medication. This morning, Matthew is spending a long time choosing his clothes. John is worried that he’ll be late to his next client. He tells Matthew to hurry up and choose something to wear, rather than constantly talking.
In this situation, John could talk to the care co-ordinator, or whoever schedules care visits in his organisation, to ask whether Matthew could have longer care visits.
Personality clashes
Care providers might not like to admit it, but not all carers and clients are a perfect fit.
Some people won’t get along easily, and this might impact on the care that clients receive.
Example:
Ray’s wife died in a motorbike accident, and Ray is vocal about his dislike of motorbikes. His carer Aimee rides a motorbike to work every day, and Ray knows this. He complains about her bike during every care visit, and Aimee finds it hard to stay patient and listen to him.
Aimee could talk to her manager about the personality clash with Ray. They might choose to schedule another carer for Ray’s care visits. Alternatively, she could talk to Ray about why his comments upset her, or work on techniques such as mindfulness, so that she feels more able to cope with Ray’s complaints.
Poor training
A care worker might be a compassionate person, but struggle to do their job because of poor training.
If they don’t understand how to carry out a certain task, or don’t feel confident supporting clients, they may not deliver the best care possible.
An otherwise compassionate carer may not even realise what they’re doing. For example, a care worker may be unaware of a client’s religious customs, and unintentionally cause offence by offering a forbidden food or breaking modesty rules.
Poor training is most commonly an issue for new and inexperienced carers, or in small organisations without a comprehensive onboarding programme.
Example:
Mina is an activity support worker, helping a variety of clients, including George, who is autistic. Mina has never worked with autistic people before, and she is worried about how to interact with George. She tries to spend more time with other clients, and less time talking to George.
In this situation, Mina should notice that she’s avoiding George and ask herself why. She could ask for extra training in working with autistic people, or ask colleagues how George prefers to communicate. Ideally, Mina’s supervisor should also notice her behaviour, and step in before it becomes a problem.
External stresses
Care workers have lives away from work, and it’s natural that they will be stressed or anxious sometimes.
Unfortunately, these worries can affect their mood when they’re delivering care for clients.
A good carer should always try to put their personal life to one side and focus on their client. However, this isn’t always possible, and sometimes care workers under pressure aren’t as compassionate as they could be.
Example:
Leah is a carer and a single mum. Before she left for work this morning, her son told her about an expensive school trip. She’s preoccupied all day with money worries, and doesn’t give her clients her full attention.
There isn’t always an easy solution for external stresses. Leah could talk to her line manager and ask for some annual leave if she’s struggling to focus. She might need to ask her GP to sign her off work for a short time. If the organisation has an Employee Assistance Programme, Leah’s manager should explain how she can access it.
Burnout
Being a care worker can be difficult, both physically and mentally.
Most carers have to deal with high levels of responsibility, challenging behaviour from clients, and even bereavement. For some care workers, this can lead to burnout.
Burnout might involve physical symptoms, such as fatigue, insomnia, pain or digestive problems. It also often includes changes in mental health, like anxiety, depression, feelings of hopelessness, and irritability. Some people find that they struggle to talk to others, or that they don’t care about other people’s problems any more. All of this can make it hard for carers to show compassion to their clients.
Example:
Two of Arlene’s long-term clients have recently died after long illnesses. She was involved in their end of life care, and worked extra hours to support them in their final days. She still has a busy schedule of care visits, but she’s finding it difficult to manage. She feels irritable and struggles to laugh and joke with her clients like she did before.
In this situation, Arlene may need to take some time away from work to recover. She could use annual leave or be signed off work by her GP.

How to improve compassion in social care
As a care manager, how can you help your team be more compassionate?
If you’ve noticed that your care team isn’t always as compassionate as they should be, consider why. Is their lack of compassion caused by time constraints, poor training, or burnout? Understanding the reasons behind their actions is key to improving compassion.
Some tactics to improve compassion among your care staff might include:
- Recruiting the right people
- Setting an example from the top
- Getting the training right
- Making time for clients
- Working together to support clients
- Supporting your staff
Recruiting the right people
Some people are naturally more compassionate and understanding. Where possible, it’s important to look for these qualities when recruiting.
How to recruit the right care staff:
- Involve clients in the interview process, so you can see how candidates interact with them.
- Collect references from previous employers, as well as character references where possible.
- Avoid rushing the recruitment process. It may be better to use agency staff than to hire the wrong person.
Setting an example from the top
As a manager or director, your team will look to you as an example. You should create a culture of compassion and kindness.
How to set an example of compassion:
- Spend time with clients yourself, and ensure that they know they can come to you with concerns.
- Always be respectful of your clients and their families. Avoid gossiping about them, or speaking badly of them.
- Act quickly if you notice staff members treating clients or colleagues poorly or engaging in discrimination.
- Normalise taking time off work when necessary. This includes sick leave, as well as maternity, paternity, or shared parental leave, compassionate leave, and your holiday allowance.
- Reward the right behaviour. Consider arranging staff awards for compassion and kindness, or otherwise recognising team members who consistently do the right thing.
Getting the training right
Care workers need to have the right skills and knowledge to support their clients.
Poor training can lead to a lack of compassion, even in otherwise kind and caring professionals.
How to train your staff team well:
- Make sure that your team are all up-to-date with their mandatory training.
- Encourage your carers to take extra training in relevant areas that interest them, such as dementia, autism, or sign language.
- Use care management software to track your team’s training. PASS includes easy-to-build employee checklists, which can help you keep on top of training and refresher deadlines.
Making time for clients
Many service users are quite isolated. They need more companionship – but care workers are often hampered by not having enough time for their clients.
Making sure that clients have enough social interaction can be a real act of compassion.
How to make time for clients:
- Ensure that care calls are long enough for support workers to deliver personal care and spend time talking to clients. Your care planning software can help you with scheduling.
- Make yourself available to clients and their families. Ensure that they know how to raise concerns or ask for a review of their care.
- Arrange social events so that your clients get to know each other.
Working together to support clients
If a client receives support from multiple carers, they should work together to provide compassionate care.
This should start with the care assessment process, and continue throughout the client’s time with your service.
How to work together to support clients:
- During your initial assessments, find out as much as you can about each client, so you can schedule the best carers for their visits – for example, carers with shared interests, specific expertise, or speakers of a particular language.
- Encourage your team to notice even small changes in a client’s health or behaviour, so they can spot potential concerns and take action.
- If you work in a care home or other residential facility, hold handover meetings at the start of each shift, so that your team can share vital client updates with colleagues.
- If you provide domiciliary care, use home care software to record details about service users, so that everyone knows about their changing needs and preferences.

Supporting your staff
Burnout, external stresses, and health concerns can all make it difficult for your staff team to be compassionate.
Unfortunately, you can’t eliminate all of these problems – but you can encourage your team to talk about their concerns, and take time to recover.
How to support your staff to be compassionate:
- Hold regular development reviews with your staff team. Ask about their work and encourage them to be honest about any worries. Make sure you follow up on their concerns.
- If your organisation uses an Employee Assistance Programme (EAP), make sure that your team know how to access it. If you don’t already use an EAP, consider signing up for one.
- Check in with staff members who are doing particularly difficult work – for example, people who support clients with challenging behaviour, or those providing end of life care.
- Where possible, avoid calling team members on their days off, or changing schedules at the last minute.
- Encourage team members to take time off when they need it.
Conclusion: what is compassion in health and social care?
As a care provider, you should make an effort to be compassionate towards all of your clients – as well as their families and your colleagues. Make sure that you treat clients with patience, kindness and respect.
Take time to understand their feelings and preferences, and avoid letting your personal stresses affect the care you deliver.
Book a free tour
Deliver compassionate care, without the admin burden
See how PASS helps you plan care, support your team, and stay connected, so nothing gets missed and every person feels heard and respected.